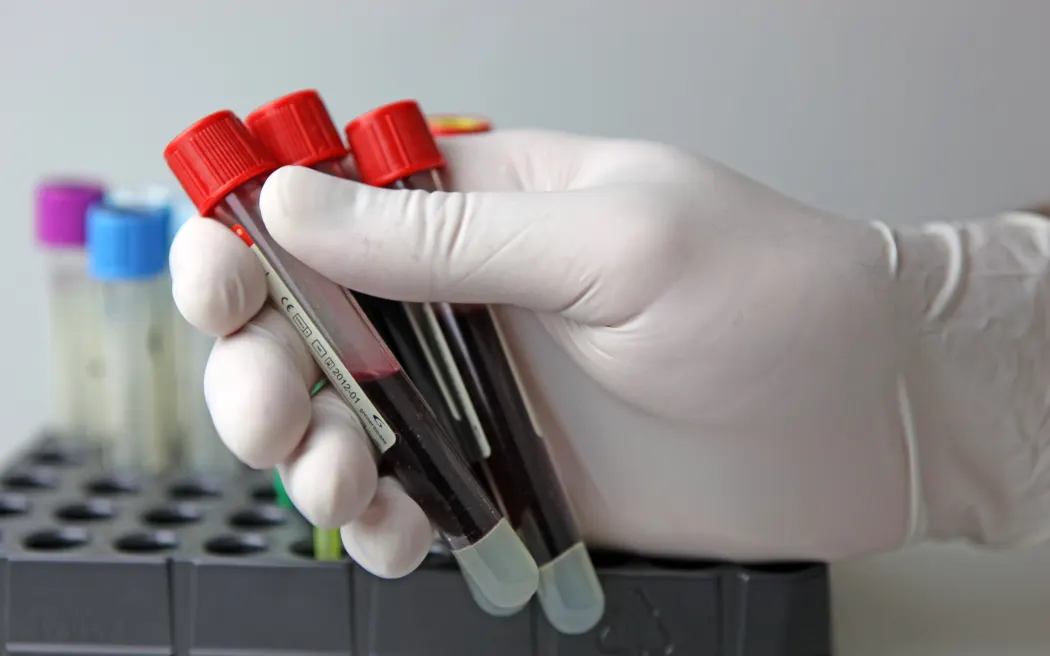
A recent UNAIDS report has revealed a dramatic rise in HIV infections in Fiji, showing that the number of people living with the virus has increased tenfold in just a decade. The 2025 Global AIDS Update: AIDS, Crisis, and the Power to Transform estimated that fewer than 500 people were living with HIV in Fiji in 2014. By 2024, that figure had surged to approximately 5,900. Despite this rise, only 36 percent of those infected were aware of their HIV status, and just 24 percent were receiving antiretroviral treatment.
The same report included testimony from Kalesi Volatabu, founder of DrugFree World Fiji, who cited preliminary 2024 data from the Ministry of Health showing that half of those newly diagnosed with HIV and receiving treatment had contracted the virus through shared needles. In response to the growing crisis, the Fijian government declared an HIV outbreak in January 2025. An HIV Outbreak Response Plan was announced alongside a broader Counter Narcotics and HIV Surge strategy, both of which call for the introduction of harm reduction programs, including needle and syringe distribution for people who inject drugs. Although these programs have received support in principle, implementation has proven challenging due to a mix of logistical, political, and cultural barriers.
Volatabu stressed that harm reduction must go hand-in-hand with education, not just about safe practices, but also about dispelling the myths and stigma that still surround HIV in Fiji. She argued that awareness must begin with leadership. “When the indigenous chiefs call, people will follow,” she said. “Then there are the churches. Last but not least, the government.” Her call to action highlights the importance of community influencers in shifting public attitudes and encouraging engagement with health services.
Fiji’s situation reflects broader concerns seen across the Pacific region, where HIV infection rates are rising amid constrained public health systems, limited access to testing, and widespread stigma. These challenges create a dangerous environment in which the virus can spread largely undetected and untreated. In countries with similar profiles, introducing needle-syringe programs alongside education and testing initiatives has significantly reduced transmission rates, especially among people who inject drugs. Global studies suggest that these programs can reduce infection by up to 80 percent when combined with counseling and access to antiretroviral therapy.
The low rates of diagnosis and treatment in Fiji are particularly concerning. When individuals do not know their HIV status, they are more likely to transmit the virus unknowingly. Untreated HIV also leads to a higher viral load, which increases transmission risks. Closing this gap is a public health priority, and one that requires an urgent scale-up in testing services and public awareness.
The key to addressing this crisis lies in a coordinated, multi-pronged approach. Expanding access to voluntary testing and counseling, fast-tracking needle-syringe program implementation, empowering community leaders to speak out, increasing treatment coverage, and launching public campaigns to reduce stigma are all critical steps. If these are taken seriously and supported at both national and grassroots levels, Fiji has the opportunity to regain control of the outbreak and prevent further escalation.
With the right strategies in place, the country can move from crisis response to long-term prevention and care. The choices made now—by government, by civil society, and by community leaders—will determine the direction of Fiji’s fight against HIV for years to come.