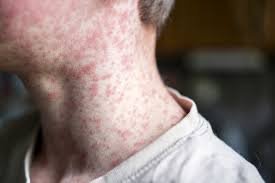
In early 2025, Morgan Birch from Alberta was alarmed when her four-month-old daughter, Kimie, developed a fever and rash. Assuming it was a minor reaction to immunisations or perhaps chickenpox, Birch sought advice from her 78-year-old grandmother. The response was unexpected and chilling—her grandmother immediately recognized it as measles.
Lab tests confirmed the diagnosis. Kimie had contracted measles, likely during a routine hospital visit in the Edmonton area. Tragically, she was too young to receive the measles vaccine, which is typically given from 12 months of age in Alberta.
Kimie’s case is one of more than 3,800 reported in Canada in 2025. That number far exceeds the measles cases reported in the United States this year, despite Canada having a significantly smaller population. According to the Centers for Disease Control and Prevention, Canada is now ranked eighth globally in countries with the highest number of measles cases, and is the only Western country on that list. Alberta currently has the highest per capita measles rate in North America.
This situation has shocked many in a country where measles was declared eliminated in 1998. The current outbreak marks the worst resurgence of the disease in Canada since 2011, when approximately 750 cases were reported. Now, the country is grappling with the question: how did measles return so fiercely in a nation with free healthcare and widespread vaccine access?
The first signs of the outbreak appeared in late 2024. In Ontario, health authorities linked the spread to an individual who contracted measles during a large Mennonite gathering in New Brunswick. The person returned to southwestern Ontario, unknowingly bringing the virus into a vulnerable community.
The virus spread rapidly within Low German-speaking Mennonite communities, where vaccination rates are historically lower due to religious and cultural views. Many members of these communities avoid modern medicine unless absolutely necessary, and vaccination hesitancy remains a challenge. Public Health Ontario confirmed that almost all of those infected in this area were unvaccinated.
Catalina Friesen, a healthcare worker serving the Mennonite population near Aylmer, Ontario, recalled the moment she encountered the first signs of the outbreak. A woman and her five-year-old child came in with symptoms resembling an ear infection, which later turned out to be measles. She said it was the first time she had ever seen measles in her community.
The virus spread quickly, with Ontario reporting more than 200 new cases per week by the end of April. While the rate of new cases has since slowed in Ontario, Alberta has emerged as the new epicentre. There, health officials struggled to identify where the outbreak began. Dr. Vivien Suttorp, a senior public health officer in southern Alberta, described the situation as the worst she has seen in her 18 years of service.
Friesen noted that Canada has a larger population of conservative Mennonite groups than the U.S., which may partially explain the higher infection rates. However, she emphasized that the community is not monolithic. Many Mennonites do support vaccinations, but misinformation has spread rapidly since the COVID-19 pandemic. She said that social media and hearsay have amplified fears about vaccine safety, particularly in communities that already feel marginalized by the healthcare system.
Vaccine hesitancy is a growing issue across Canada, not just in isolated communities. According to experts, routine vaccination rates have declined since the pandemic. In southern Alberta, the number of MMR (measles, mumps, rubella) vaccinations administered dropped by nearly 50% between 2019 and 2024.
During the pandemic, vaccine mandates led to major protests, such as the Freedom Convoy in Ottawa, where demonstrators camped in the capital for two weeks in 2021. Since then, opposition to COVID-19 vaccines has spilled over to other immunisations, including those required for children.
Dr. Janna Shapiro, a postdoctoral fellow at the University of Toronto’s Centre for Vaccine Preventable Diseases, said that outbreaks like this often begin by chance, when an infected person introduces the virus into a population with low immunity. Once measles finds a vulnerable group, it spreads rapidly. She emphasized that the only long-term solution is increasing vaccination coverage.
The case of baby Kimie highlights how quickly measles can harm those who have no protection. Kimie is recovering, but doctors continue to monitor her for possible long-term effects such as pneumonia or encephalitis. Her mother, Morgan Birch, said she felt not only horrified but also angry when she discovered what had happened. She called on fellow parents to vaccinate their children and protect those who are too young or too vulnerable to do so themselves.
In response to the outbreak, Alberta has lowered the minimum age for the first measles vaccine dose. Health authorities across the country have also launched public awareness campaigns through radio ads and bulletins to encourage immunisation. However, public response has been subdued compared to the heightened urgency during the COVID-19 pandemic.
Experts say the 2025 measles resurgence should serve as a wake-up call. Even in a country with universal healthcare, the erosion of trust, spread of misinformation, and gaps in community engagement can create ideal conditions for outbreaks. Canada’s experience this year underscores the fragility of public health victories and the importance of continued vigilance in the fight against vaccine-preventable diseases.